Study participants
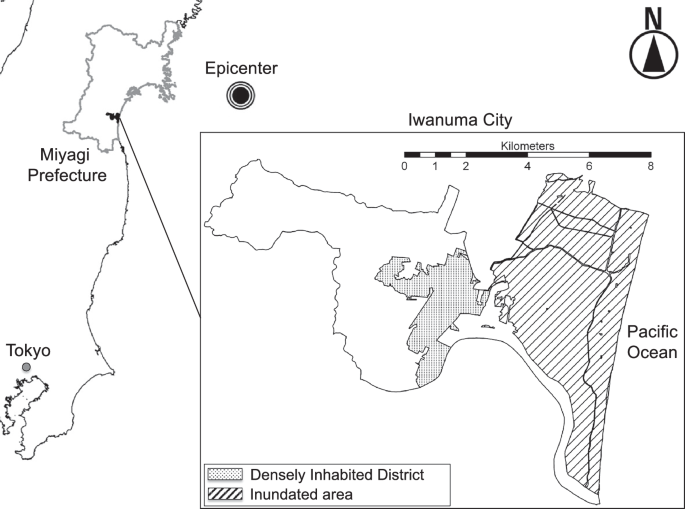
The Japan Gerontological Evaluation Study (JAGES) was launched in 2010 to investigate the health and lifestyle of adults aged 65 years or older across Japan. One of the study’s field sites was located in Iwanuma City, Miyagi Prefecture, which had a total population of 44,187 in 2010 and was severely affected by the 2011 Japan Earthquake and Tsunami. The city recorded 180 deaths, 5542 damaged homes, and flooding over 48% of its land area (Fig. 1). Seven months before the disaster (August 2010), questionnaires were mailed to all older residents using the city’s residential registry (n = 8576). The survey collected detailed information on personal characteristics, lifestyle, and health, with a response rate of 59.0% (n = 5058), comparable to other surveys of community-dwelling older adults16. Baseline data were subsequently linked to municipal records of annual health check-up participation and to the Japanese Long-Term Care Insurance (LTCI) database, which provided longitudinal information on the incidence of cognitive decline among baseline participants through December 31, 2016.

Administrative boundaries were processed from the National Land Numerical Information (MLIT, Japan; CC BY 4.0). Densely Inhabited Districts (DID) were processed from the National Land Numerical Information (MLIT, Japan; commercial use permitted). Tsunami inundation areas were processed from the Reconstruction Support Survey Archive, City Bureau, MLIT (Japan; free use including commercial purposes).
We conducted follow-up surveys of survivors in November 2013 and November 2016. The 2013 survey uniquely included questions on disaster experiences, in addition to lifestyle and health information, whereas the 2016 survey focused primarily on health status and lifestyle factors. These follow-up data were merged with the baseline dataset to create an unbalanced panel (3492 and 3195 respondents in the 2013 and 2016 surveys, respectively). To minimize sample loss and mitigate completion or survivorship bias, we avoided restricting the analysis to complete cases and retained all available person-year observations.
Respondents with invalid identification numbers (n = 10) and those who had already developed cognitive decline by the date of the disaster (March 11, 2011; n = 297) were excluded from the analysis. The final analytic sample, therefore, included 4751 participants.
Participants were followed from March 12, 2011, through December 31, 2016 (1815 days in total). Person-year observations occurring after the first diagnosis of cognitive decline were censored and excluded from the long-format dataset to avoid counting post-outcome time. Follow-up ended at the first occurrence of certified cognitive disability, death, or out-migration, and person-time after these events was not included in the long-format dataset.
The survey protocol was reviewed and approved by the Ethics Committees on Research of Human Subjects at the Harvard T.H. Chan School of Public Health (23143), Tohoku University (21-40, 24-29), Nihon Fukushi University (10-05, 13-14), and Chiba University (2493). Each respondent provided written informed consent to participate in the study.
Explanatory variable
The explanatory variable was municipal health check-up attendance, obtained from municipal administrative records for each year between 2010 and 2016. All older residents were eligible for one municipal health check-up per fiscal year, scheduled in June, July, or November and provided through local health clinics and the public health center. The fee was 1500 JPY (roughly USD $10 at current exchange rates) for those aged 65–74 years, whereas it was free for those aged 75 years or older. For each fiscal year, we defined a binary indicator of municipal health check-up attendance (1 = attended the municipal health check-up; 0 = did not attend).
In the person-year dataset, this indicator was updated annually, and a one-year lag was applied so that health check-up attendance in year t − 1 corresponded to the incidence of cognitive decline in year t.
Outcome variable
The outcome was cognitive decline, identified using data from the Japanese Long-Term Care Insurance (LTCI) database. Since 2001, the Japanese government has operated a national insurance system for older adults requiring long-term care (e.g., in-home assistance with daily activities such as house cleaning, meal preparation, bathing, etc). In order to determine eligibility for long-term care, trained assessors are dispatched to individuals’ homes in order to evaluate cognitive function (e.g., short-term memory, orientation, and communication abilities) as well as mental and behavioral symptoms (e.g., persecutory delusions and confabulation) using a standardized protocol during in-home assessments12. Based on these evaluations, applicants are classified into one of seven levels of cognitive disability, ranging from level 1 (mild cognitive deficits but largely independent) to level 7 (requiring continuous medical care in a specialized facility) (Table S1)17.
This index of cognitive decline has been shown to be strongly correlated with the Mini-Mental State Examination (Spearman’s ρ = 0.73, p < 0.01)18. Level 1 on this scale roughly corresponds to a Clinical Dementia Rating (CDR) score of 0.5, with both sensitivity and specificity of 0.8819. For analysis, we used a binary outcome with a cut-off at level 2, indicating loss of independence in daily life due to cognitive impairment—characterized by frequently getting lost in familiar areas or making noticeable mistakes in tasks previously managed independently, such as shopping, personal administration, or financial management20,21.
Covariates
We selected 40 potential confounders from the three survey waves, including four demographic characteristics (age, sex, marital status [divorced or bereaved], and living alone); three socioeconomic characteristics (educational attainment, equivalized household income, and employment status); 14 health conditions (activities of daily living, a higher risk of depressive symptoms [≥5 points on the Geriatric Depression Scale–15]22, and current treatment for medical conditions including cancer, heart disease, stroke, hypertension, diabetes, hyperlipidemia, musculoskeletal disorders [e.g., osteoporosis, arthritis], injury or fracture, respiratory disease, visual impairment, hearing impairment, and gastrointestinal, liver, or gallbladder diseases); 13 psychosocial factors (receiving and providing emotional support; receiving and providing instrumental support; frequency of participation in volunteer or sports clubs; frequency of meeting friends; number of friends met in the past month; daily social interaction with neighbors; having a hobby; expectations for mutual help in the local community; trust in local residents; and attachment to the community); and six behavioral factors (current smoking, current alcohol drinking, frequency of eating meat or fish in the past month, frequency of eating vegetables or fruits in the past month, frequency of going out, and daily walking time) (see also Table S2).
We also included housing damage caused by the disaster as a potential confounder and effect modifier. In the 2013 survey, respondents retrospectively reported the level of housing damage, which had been formally assessed by property inspectors. Damage was classified into five categories: 1 = no damage, 2 = partial damage, 3 = minor damage, 4 = major damage, and 5 = complete destruction.
Covariates measured in 2010 were carried forward to 2011–2012, and those measured in 2013 were carried forward to 2014–2015. Disaster-related variables collected in 2013 were not carried forward. This pragmatic approach ensured the use of the most accurate and contemporaneous information available for each period.
Statistical analysis
We implemented the Augmented Inverse Probability Weighting (AIPW) method to estimate both the Average Treatment Effect (ATE) of health check-up attendance on cognitive decline and the Conditional Average Treatment Effect (CATE) across subgroups defined by housing damage levels.
The AIPW estimator integrates information from the treatment model, which estimates the time-varying probability of attending annual health check-ups, and the outcome model, which predicts the incidence of cognitive decline. This approach offers double robustness, such that consistent estimates can be obtained even if one of the two models is misspecified23. In addition, both models incorporated the same set of 40 covariates and calendar-year indicators to adjust for secular time trends and potential changes in health check-up practices.
To minimize potential bias arising from model misspecification, both components were estimated using the ‘SuperLearner’ R package, an ensemble machine learning algorithm24. The candidate library comprised regularized regression (implemented via the ‘glmnet’ package), random forests (‘ranger’ package), and Bayesian generalized linear models (‘arm’ package).
Standard errors and 95% confidence intervals were calculated using a cluster-robust variance estimator based on the influence function, accounting for repeated observations within individuals.
To address potential bias arising from differential follow-up and non-response, two sets of inverse probability weights were estimated separately and then multiplied. First, inverse probability of censoring weights (IPCW) were derived from a logistic regression model predicting the probability of remaining uncensored, defined as not experiencing a competing event such as death or relocation, based on baseline covariates including age, sex, educational attainment, income, marital status, employment, and depressive symptoms, as well as calendar year25. Second, inverse probability weights for survey response were obtained from a corresponding logistic model predicting the likelihood of responding to each survey wave using the same covariates and calendar-year indicators26.
As a sensitivity analysis, we conducted age-stratified AIPW analyses to examine the association between municipal health check-up attendance and cognitive decline separately for participants aged 65–74 years and those aged ≥75 years at baseline, using the same covariate set as in the main analysis. This analysis was motivated by the fee waiver for municipal health check-ups among individuals aged ≥75 years and was intended to examine whether the estimated effect differed by eligibility for free check-ups.
We also conducted another sensitivity analysis restricted to address potential left truncation; we repeated the main analysis in the subgroup of respondents who reported never having participated in any health check-ups before the 2010 survey.
Across all analyses, we calculated E-values for the risk ratio point estimates and for the confidence-interval limit closest to the null in each exposure–outcome association, in order to evaluate the robustness of our effect estimates to unmeasured confounding. The E-value quantifies the minimum strength of association that an unmeasured confounder would need to have with both the exposure and the outcome, conditional on the measured covariates, to fully explain away the observed exposure–outcome relationship27.
Missing data were imputed using a random forest algorithm implemented in the ‘missForest’ package in R28. All analyses were conducted using R version 4.5.0 (R Foundation for Statistical Computing, Vienna, Austria).
link